|
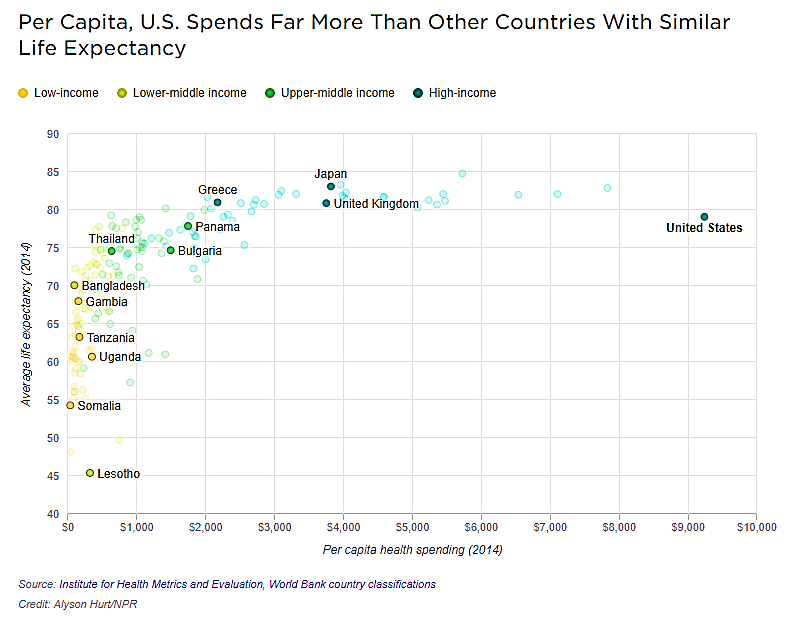
The United States (US) spends more on healthcare for its citizens than any other country in the world. Healthcare expenditures are approximately 17.9% of the gross domestic product
[1]; however, dollars spent are not necessarily translating into better health outcomes, better quality of life or longer life expectancy compared to countries that spend less. This is best exemplified when examining life expectancy in the US versus Japan, both developed, high income countries. The life expectancy in the US is 79.1 years, whereas the life expectancy in Japan is 83.1, and Japan spends ($4,519 in 2016
[2]
) consi
derably less than the US ($10,348 in 2016[2]) on healthcare.
[3]
In contrast to he
a
lthcare spending, the U
S has spent approximately 3% of the health budget on public hea
lth activities.
[4]
It is important to note the difference in spending considering that dollars spent on prevention and population health greatly improve the health status of communities and result in impressive health care cos
t savings. For example, p
ublic health programs that add
re
ss healthy eating, physical activity, and lifestyle changes can help deter the onset of chronic diseases such as diabetes, obesity, and cardiovascular disease (CVD),
which in turn can reduce the financial burden of disease and prevent loss of productivity.
Why does this matter to Indian Country?
A small portion of federal government spending goes towards public health efforts and an even smaller portion of that goes towards the health and wellness of American Indian and Alaska Native (AI/AN) communities. Public health strategies can prevent illness and injury in AI/AN populations, promote a better quality of life, and reduce strain on an overstretched Indian health care system. Investing in Tribal public health can address health disparities ex
perienced by AI/AN people such as: diabetes, CVD, cancer, substance misuse, and suicide - some of the leading
causes of death in I
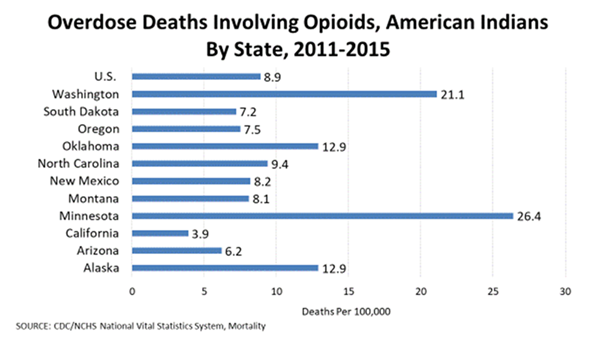 ndian Country. For example, AI/ANs experienced the highest drug overdose deaths by race every year from 2008 to 2015, and the highest percentage increase in overdose deaths by race at 519% from 1999 to 2015. The death rate for chronic disease such as diabetes is 34.1 in Indian Country compared to 18.1 for non-Hispanic Whites in 2013
[5]
. Investing in public health is a viable way to improve health outcomes and address the health disparities experienced by AI/ANs.
ndian Country. For example, AI/ANs experienced the highest drug overdose deaths by race every year from 2008 to 2015, and the highest percentage increase in overdose deaths by race at 519% from 1999 to 2015. The death rate for chronic disease such as diabetes is 34.1 in Indian Country compared to 18.1 for non-Hispanic Whites in 2013
[5]
. Investing in public health is a viable way to improve health outcomes and address the health disparities experienced by AI/ANs.
Trust responsibility and public health
The federal government took on an obligation to provide healthcare to Tribes through treaties, and later re-affirmed those duties in Supreme Court case law, legislation, and executive orders. Federal agencies such as the Indian Health Service (IHS) have partially fulfilled this responsibility by funding approximately 50% of the need in Indian Country. Some estimates demonstrate a much smaller percentage of need is met. What is readily apparent - unmet needs must be addressed, the federal government must uphold its obligation to Tribal Nations, and a public health approach offers excellent opportunities for positive impact.
Protecting the health of all American citizens, requires a substantial and sustained investment in Tribal public health. Disease outbreaks and public health emergencies in AI/AN communities impact the entire Nation. There are no borders or boundaries that will keep illnesses and outbreaks in one community from reaching others. Ensuring the federal government fulfills its responsibility to Indian Country includes making prevention and
public health the center of healthcare. This will not only aid in reducing healthcare costs, but will also prevent chronic disease and outbreaks - benefiting all communities.
|
|
|
|
|
|