Note: New Content Noted with Asterisks*** and Highlighted
Dear KHF Providers and Practice Administrators,
We have several updates to share regarding payor updates, programs and upcoming events. There is a lot of information, and we want to make sure we are keeping our membership informed. We recommend reading through this communication in its entirety and please reach out to us with any questions you may have!
| |
***Important: Update on K1's***
We are incredibly sorry that K1’s have been so late this year and appreciate everyone’s patience. We have been in daily contact with the new Accountants about it and they have been working on them. We realize the importance of getting these to you timely so that you can complete your partner accounting and then do individual tax returns. We are already working on plans for next year so this does not happen again.
- The IPA-GA Liability Program LLC K1’s were sent out 4/6/23 by Shatell – please let Barbara know if you did not receive the email yet.
- The IPA-Greater Atlanta, LLC K1’s should be sent on Monday – as soon as we get them we will email them to you.
| |
***Upcoming Virtual PA Meeting- Active Shooter Training***
This is a reminder that the Practice Administrators Meeting will take place on Thursday, April 20, 2023, at 10:00am – 12:00pm via Zoom.
Joining us for the meeting will be Zachary Williams, Protective Security Advisor with the Department of Homeland Security to discuss employee and office security during an active shooter type event.
To Join the meeting:
https://us02web.zoom.us/j/81036277397?pwd=dmZEV0NJSThUUThPN2RlWUZLb0I5Zz09&from=addon;
Meeting ID: 810 3627 7397; Passcode: 429112.
Please, RSVP by replying to this e-mail.
| |
IPA-GA Committee & Board Recruitment
To KHF Physicians:
If you are interested in being part of the Quality/Utilization Management Committee or the IPA-GA Liability Program Board of Directors and would like more information, click on the link to leave your name and contact information.
Quality/Utilization Management Committee:
- Reports to the Board of Managers, serves as Board’s steward for overall quality improvement of the network
- Goals are to maintain the highest possible standards of practice that will improve the health outcomes of its members, promote accessibility and cost-effective quality care
- Provides oversight of network standards, monitoring adherence to those standards, makes recommendations for improvement
- Leads development of clinical practice and referral guidelines and potential Maintenance of Certification (MOC) programs
- Meeting frequency: Quarterly, mainly virtual, in person if needed
IPA-Ga Liability Program Board of Directors:
- Practice must be a participating member
-
Tasked with financial oversight of the program, oversight of program policies and procedures and managing any claims
- Meeting frequency: Quarterly, virtual, usually 30-60 minutes
| |
DEI-Focused Clinical Quality Forum Recording
Thank you to everyone who attended last week’s virtual Clinical Quality Forum. We had 140 attendees, which is one of our highest turnouts and a great start to our programming for the year! If you haven’t had the chance to complete the short evaluation survey, please click here and let us know what you thought of the program.
This module was the official kick-off for our member-facing Diversity, Equity, and Inclusion strategy, and we hope that the education on equity, the compelling parent interviews touching on medical bias, and the deeper dive into the clinical impact of social determinants of health on asthma and other chronic diseases give some context for TCCN’s broadened focus on DEI in our quality program. We look forward to digging into these topics with you all and discovering additional opportunities to further equitable patient care.
If you were not able to attend live, we highly encourage you to watch the recording and complete the attestation via this link or the QR code above to receive your TCCN participation credit. The recording is roughly 1 hour. If you attended live, there is no further action needed for your practice to receive credit. One least one provider from each practice must view this program or the upcoming Fall Clinical Quality Forum. In addition, each practice must view the short DEI educational video that was at the beginning of the module, so your participation for this program will fulfill two of your 2023 requirements.
We are gathering answers to a few questions that were put in the chat and will send those out in the next follow-up email for this event. If you have any additional questions related to this content, please let us know as soon as possible so those can be incorporated.
| |
Benchmarking Request - practice survey - due 4/28/23
Dear Practice Administrators and Lead Physicians,
We want to thank you for your cooperation and participation in our benchmarking program thus far. The information you provide helps us continue to analyze aggregate data at a network level and spot trends that are affecting our practices.
Here is a blank copy of the 2023 Practice Benchmarking Survey. All information will be based off of calendar year 2022 data. To assist you in completing the survey, here is a word document with detailed instructions to guide you through the Benchmarking worksheet. The attached Benchmarking worksheet consists of a total of 11 tabs, but remember, you only have to complete the cells that are highlighted in yellow! As with all of our Benchmarking requests, the provided information will remain strictly confidential.
The deadline for returning the surveys is April 28, 2023. Please return your completed survey to Elizabeth Hogan at [email protected]. The results will be returned via email on or before the May or June Practice Administrator meeting.
The Board of Managers and Kids Health First appreciates the time it takes from your busy schedules to participate in the Benchmarking initiative. In addition to the valuable data your practice gets from participating, the Board is offering a $50 Amazon gift card to practices that complete the practice survey on time.
A great value that Kids Health First can bring to our members is Benchmarking data. Please take your time when completing the survey to ensure the data is accurate. Feel free to contact me if you have any questions. We appreciate all of your hard work and want to thank you again for another successful benchmarking season!
| |
According to the AAP, some Gerber infant formula has been recalled due to possible bacteria contaminant. To learn more, click here.
This article from the FDA, has updated the information and lists out the items which have been recalled, which I have also listed below. There is also a 1-800 number which parents can call for more information:
Gerber® Good Start® SoothePro™™ 12.4 oz:
300357651Z – USE BY 04JUL2024
300457651Z – USE BY 05JUL2024
300557651Z – USE BY 06JUL2024
300557652Z – USE BY 06JUL2024
300757651Z – USE BY 08JUL2024
300857651Z – USE BY 09JUL2024
301057651Z – USE BY 11JUL2024
301057652Z – USE BY 11JUL2024
301157651Z – USE BY 12JUL2024
Gerber® Good Start® SoothePro™™ 30.6 oz:
301357652Z – USE BY 14JUL2024
301457652Z – USE BY 15JUL2024
301557651Z – USE BY 16JUL2024
Gerber Good Start® SoothePro™™ 19.4 oz:
301557652Z – USE BY 16JUL2024I
Consumers can request refunds for impacted products and get more information about Gerber® Good Start® by contacting the Gerber Parents Resource Center. They are available 24/7 on behalf of Perrigo at 1-800-777-7690.
| |
Social Media Posts for Medicaid and End of PHE
To help your patients and families better understand the end of Public Health Emergency and the unwinding of Medicaid, and what it may mean to them, please feel free to post these on your social media platforms. For more information, visit
for additional Questions and Answers they may have, visit the Kids Health First communication resource page.
| |
News from the AHA related to the PHE and Medicaid
On Friday, March 17th, 2023 the American Hospital Association posted the following news from the HHS and the Kaiser Family Foundation on emergency use authorization in light of the coming end of the PHE, and the recent survey on states approach to ending the continuous enrollment on March 31st and how it will impact Medicaid and CHIP recipients. Please see below for the information.
HHS: FDA COVID-19 emergency use authorizations remain in effect
Health and Human Services Secretary Xavier Becerra this week amended the February 2020 COVID-19 emergency use authorization declaration so that the Food and Drug Administration’s emergency use authorizations for COVID-19 diagnostics, personal protective equipment, other medical devices, and drug and biological products will remain in effect until there is no longer a “significant potential” for a COVID-19 public health emergency or the authorized devices or products have been approved. For more information, see the FDA’s EUA questions and answers.
Survey looks at state approaches to renewing Medicaid, CHIP enrollments
The latest annual survey of state Medicaid and Children’s Health Insurance Program directors by the Kaiser Family Foundation and Georgetown University Center for Children and Families looks at state approaches to renewing Medicaid and CHIP enrollments over the past year and once the COVID-19 public health emergency’s continuous enrollment requirement ends on March 31. According to the January survey, all states have encouraged enrollees to update their contact information; 43 states have continued to process ex parte renewals over the past year; 41 states are engaging managed care organizations to help with renewals; and 35 states are prioritizing renewals based on factors such as time since last renewal and potential ineligibility. More than two-thirds of states said they have extended or plan to extend postpartum coverage for a full 12-months post pregnancy.
| |
|
Communication #1-Stay tuned for updates
The End of the Public Health Emergency (PHE) for COVID-19: What does that mean for me and my family?
On January 30, 2023, the White House announced its plans to end the coronavirus public health emergency (PHE) in May. The PHE is scheduled to end on May 11, which will result in changes that will affect the access and cost to vaccines, tests, and treatment for COVID-19. This will include changes to telehealth policies.
During the pandemic, many of you received COVID tests, vaccines and treatments free of charge. When the emergency period ends on May 11, changes will occur on the availability and cost of the above. The White House did not want to end the PHE quickly and has given both patients and providers several months’ notice to learn more about the upcoming changes.
| |
The "AAP's Bold Stance on the Value of Pediatrics"
by Allie Squires, Editor of The Independent Pediatrician
In a landmark policy statement, the AAP is stating the reasons why and how payment reforms are necessary for the future of the healthcare system. Read more.
| |
KHF Questions of the Day
Survey Results: Fluoride Treatment Questions
Survey Results: Varicella and MMR Billing Issues Survey
Has your practice noticed any EOBs where when you have billed for Varicella and MMR the payors are changing it to ProQuad and dropping the admin fee? 8 of 23 respondents said yes. Payors include BCBS, Humana, Aetna, Cigna, and UHC. Please notify [email protected] if you have this issue and haven't already.
We surveyed! You answered! Previous Surveys are below!
| |
|
Remind me, again, which of the almost 2-dozen 'telemedicine' codes can only be done by a physician (vs. a qualified non-physician)? Which ones can't be used if an E&M has been billed in the last seven days? Or if a decision is made to schedule an appointment in the next twenty-four hours?
I seriously can't remember. Fortunately, Jan Blanchard did the work for us. Check out this nicely laid out table for you and your billers. Well done! Click on it to download the pdf.
| |
|
Update from KHF and AAP on COVID Vaccines
Dear Fellow KHF Pediatricians,
As you have all heard, the public health emergency will be coming to an end on May 11, 2023. What will this mean for all of us? Many of you may have questions regarding COVID vaccines, testing and treatment moving forward. The AAP is aware of these concerns and is working at state and national levels to support pediatricians in our efforts to protect and treat our patients as the PHE ends.
Kids Health First has been an excellent source of information during the pandemic and will continue to gather and disperse information to all of you so that your offices may plan for these upcoming changes which will affect all of us. Be assured that we are here to support you and will continue to send helpful information as it becomes available.
This letter from Dr. Sandy Chung is our most up to date summary.
Best Regards,
Lori Desoutter, MD
Medical Director, Kids Health First IPA
Melinda Willingham, MD
Board of Managers, Kids Health First IPA
American Academy of Pediatrics, Chair, Committee on Federal and Government Affairs
| |
TCCN is pleased to announce the signature of a contract with CareSource.
The comprehensive agreement includes base contract terms for delegated primary care members and a value-based program for all TCCN members. The agreement will have an effective date retroactive to January 1, 2023. More details will be forthcoming as we implement this new agreement.
| |
CMO State Request for Proposal (RFP) Update
As the State continues its CMO bidding process for contracts that are planned to start in 2024, you have likely noticed communications being sent to your practice by entities that are interested in entering our market with their CMO product. We are aware that the following entities may be reaching out to you:
- Aetna
- AmeriHealth Caritas
- Humana
- Molina
- UnitedHealthcare
TCCN is in discussions with several of these entities regarding potential contracting through TCCN should they be selected by the State. If your practice intends to contract with any of these entities through TCCN, you do not need to respond to these requests.
We reached out earlier this summer to request your delegation responses for the new entities. If you have not yet responded, or you are not sure, please reach out to Sahdeja Serieux. We need responses from all primary care practices, whether you participate with the CMOs or not.
We will provide additional updates as the State RFP process continues. Thank you!
| |
Anthem Contracting Update
TCCN has worked with Anthem since January 15, 2022 to resolve data issues following the contract implementation.
Anthem completed their audit of TCCN’s provider data and on March 2, 2023 initiated a claims sweep. The sweep will identify inappropriate denials and underpaid claims for dates of service 1/15/2022 to present.
The claims sweep could take up to 90 days to complete and practices may encounter recoupments as claims are reprocessed. This is especially the case for Anthem claims outside of BCBS of Georgia.
| |
Reimbursement policy update: Modifiers 25 and 57 - Professional
Mar 1, 2023 • Policy Updates / Reimbursement Policies
Effective March 1, 2023, the Modifiers 25 and 57: Evaluation and Management with Global Procedures reimbursement policy will be renamed Modifiers 25 and 57 - Professional. Additionally, the Nonreimbursable section of the Modifiers 25 and 57 policy was updated to indicate that CPT® code 99211 is not eligible for reimbursement when billed with modifier 25. This update was previously communicated in the July 2022, edition of the Provider News article titled Reimbursement Policy update: Modifier Rules – Professional:
Notification regarding reimbursement changes to COVID-19 laboratory services codes (MAC)
Beginning with dates of service on or after April 1, 2023, or the end of the public health emergency (PHE), whichever is later, reimbursement for COVID-19 laboratory service codes may be reduced for participating providers contracted with Anthem.
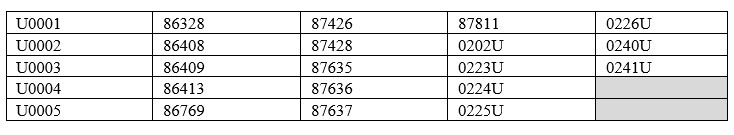
New COVID-19 laboratory service codes were implemented and reimbursed at rates to meet the needs of providers during the PHE. Reimbursement will now be revised to Anthem's standard reimbursement methodology for the following codes:
|  | |
|
Humana
Updated Provider Manual effective March 1, 2023
https://docushare-web.apps.external.pioneer.humana.com/Marketing/docushare-app?file=5028855
Introducing an online community resource directory
https://humana.findhelp.com/
Addressing health-related social needs can be important to your patient’s health. That’s why Humana Community Navigator, powered by findhelp, offers an online directory of community resources with more than 500,000 social service programs across the United States.
For any patient, no matter their insurance carrier, Humana Community Navigator can unlock resources that support your patient’s care plan, leading to better health outcomes.
- Access an easy-to-use directory of community resources at no cost to your practice.
- Offer resources in over 100 languages that are free or at a reduced cost.
- Share resources for needs such as food, housing, transportation and more!
| |
United Healthcare
New ID cards coming for some commercial plan members
Effective 4/1/2023
https://www.uhcprovider.com/en/resource-library/news/2023/new-id-cards-commercial-plans.html
Effective with date of service January 1, 2023, the Evaluation and Management reimbursement policy will be revised to align with the Evaluation and Management (E/M) CPT coding and guideline changes from the American Medical Association (AMA) and the Centers for Medicare and Medicaid Services (CMS).
Get ready to submit electronically in 2023
Reconsiderations, appeals and claims moving to digital submissions only
https://www.uhcprovider.com/en/resource-library/news/2022/paper-submissions-go-digital-2023.html
We started with transitioning mail we send you to electronic delivery. Next, we’ll shift to eliminating paper you send us.
In 2023, network (contracted) health care professionals, practices and facilities will be required to submit claim submissions, claim attachments, and reconsideration and appeal requests to UnitedHealthcare electronically. In response to feedback from members, we’ll also emphasize and encourage the use of digital ID cards for commercial plans.
We recognize that these changes are significant, so we’re alerting you early to give you more time to plan ahead. The effective dates for these incoming paper-to-digital transitions will be announced in Network News at least 90 days prior to the change.
Click the link for a preview of what to expect with these changes, as well as more information on digital ID cards for commercial members.
| |
Cigna Updates
Q1 2023 News Publication
https://editiondigital.net/publication/?m=33093&i=778935&p=2&ver=html5
Cigna has published their Q1 2023 news publication. There are several items of interest notes with page numbers below.
Page 3 – Digital ID Cards Are Here
Page 4-5 – Clinical, Reimbursement, and Administrative Policy Updates
Page 6 – Preventative Care Services Policy Updates
Page 7 - Virtual Care Reimbursement Policy
Page 9 – Webinar Schedule for Digital Solutions
Page 11-12 – Cigna + Oscar Health Plans Information with sample ID cards
Page 23 – HEDIS and QRS Data Collection Are Right Around the Corner
Additional Virtual Care Services Now Permanently Reimbursable
virtual-care-reimbursement-policy.PDF (cigna.com)
Cigna has added the following services and codes as permanently reimbursable as part of our Virtual Care Reimbursement Policy (R31).
- Quick five- to 10- minute telephone conversations between a provider and their patient: HCPCS code G2012
- eConsults: CPT codes 99446-99449, 99451, and 99452
- Virtual home health services: HCPCS codes G0151-G0153, G0155, G0157-G0158, G0299-G0300, G0493, S9123, S9128-S9129 and S9131
| |
Georgia Medicaid
Lactation Consultants – Revised Policy effective 3/15/2023
https://www.mmis.georgia.gov/portal/PubAccess.Provider%20Information/Provider%20Messages/tabId/19/Default.aspx
Spring Virtual Medicaid Fair
Save the Date: Thursday, April 20, 2023. The Virtual Spring Medicaid Fair will offer important updates on emergent issues by DCH leadership and several break-out sessions covering a variety of topics. Registration information will be posted soon. Please submit your suggested breakout topics to [email protected] no later than Friday, March 10, 2023.
Provider Messages (georgia.gov)
Medicaid Member Redetermination:
DCH has not contacted members in 2 years and will begin member redetermination outreach on February 1, 2023. They must initiate contact with all Medicaid members within 12 months and complete the redetermination within 14 months in accordance with CMS guidelines. Members will be contacted during their renewal month. For example, if a member had a historical renewal in April, they will not be contacted until April. If the member utilizes SNAP/TANF, DCH will align with those programs to only contact the member one time.
How can the provider community help?
-
Please review https://staycovered.ga.gov/ for the latest PHE Unwinding information.
-
Proactively encourage and remind Medicaid patients to update their personal information on the Gateway website: https://gateway.ga.gov/access/
-
Share video, images, and the PHE toolkit that are found on https://staycovered.ga.gov/ with your patients.
Georgia Medicaid Provider Revalidation
Provider revalidation has also been voluntary due to the PHE. However, in 2023 the revalidation will become mandatory. Gainwell is reaching out to providers to assist with the revalidation process. The Revalidation/Recredential application is one application. For providers with multiple service locations, you will be required to Revalidate each additional service location. If you are unsure of your providers revalidation dates, log into www.mmis.gammis.gov Select Providers, then Demographic Maintenance, the Revalidation Date is present. Posted on GAMMIS in Provider Notices (9/1/2022) “Presentation-Physician Services-September 2022,” (Slides 25-27)
| |
In Case You Missed It
Kids Health First Who to Call List
Here is the Kids Health First Who To Contact List. Please contact our team with any needs you may have.
2-Week Data Submission Requirement
The TCCN Board of Directors met on May 18, 2022, and revisited the initial recommendation made in 2018. At this time, by vote of the BOD (as allowed by the TCCN agreement with Network Participants), the TCCN BOD requires all practices to submit claims data to the PHM Tool within 14 calendar days of the most recent encounter date. This requirement will take effect beginning August 1, 2022. Please click here for more information.
2023 Pediatric Coding Update and Managing the Challenge of Surge
The Georgia AAP held a webinar on January 31st titled 2023 Coding Updates and how to meet the needs of your patients during a surge. In the webinar there are a few coding updates that may be applicable to your practice. Additionally there are several suggestions for managing your patient flow when there are patient demands to be seen.
Here is the link to view the recording. Passcode: u*1Xuh11
2023 Pediatric Coding Update and Managing the Challenge of Surge Slide Deck
KHF PA Meeting 2/16/23
Click here for the deck. Click here for the recording of the meeting.
1/19/23 PA Meeting Materials
Thank you for attending the PA meeting yesterday. Here is the slide deck and this is the link to the recording if you missed it.
Nov. 17th Pediatric Coding Seminar Recording and Materials
Thank you to everyone who attended our annual Pediatric Coding Seminar! If you were not able to attend, a link to the recording is provided below along with color and black and white versions of the meeting slides for your records.
2023 Pediatric Coding Seminar Recording
Slides: Color and Black & White
Free OSHA Training
Here is the link to the OSHA Webinar held on 9/15/22.
Here is the pdf of the deck.
Here is the end of course test.
If you attended the meeting live your certificate will be emailed to the email address you posted in the chat. If you were unable to attend live and you watch the video above and complete the test and would like your certificate of completion, please email Tandric Bowden at [email protected].
Georgia DPH: Meningococcal Conjugate Vaccine Requirement
The Georgia Department of Public Health has published a letter to all providers regarding administration of the meningococcal conjugate vaccine (MenACWY). Please read the letter here for the full details and contact the Georgia Immunization Program if you have questions.
Monkeypox Q&A for Parents
Please click here for the Q&A KHF developed with our Medical Director Dr. Sally Marcus.
Q&A for Parents/COVID-19 Vaccine for Children Under the Age of 5: The Centers for Disease Control and Prevention’s (CDC) Advisory Committee on Immunization Practices met June 17-18, 2022, to discuss the FDA recommendations on the emergency use (EUA) authorization of the Pfizer-BioNTech and Moderna COVID-19 vaccines in children between 6 months thru 5 years of age. We have created an important FAQ for practices as a resource for parents who may have questions.
Q&A for Parents:The Bivalent COVID-19 Vaccine for Children 5 years and Older
Please click here for a Q&A KHF has put together that you can distribute to your patient's parents regarding the bivalent COVID-19 vaccine.
| |
|
Communications:
TCCN Roundup:
The TCCN Roundup is designed to be a twice weekly information hub for all things TCCN.
-
Please to check out the latest issue.
- Please note that the link above only accounts for some TCCN updates. In order to view the full TCCN Newsletter with your contracted payor updates please check your TCCN inbox!
TCCN Quality Steps Newsletter
| | | | |